Having been overweight as a child and through most of my adolescence, I can relate to not only the frustration of ill-fitting clothing and lack of interest in physical activity, but also how easy it is for a young person to feel helpless when it comes to getting into shape and being healthier. (Sadly, many parents don’t fully understand the basics of nutrition on a practical, everyday level enough to pass on good habits to their kids.)
From experience having worked at a summer fitness camp (aka “fat camp”) as an adult, I’ve seen the yo-yo cycle of kids eating right and getting exercise during the summer away from home, only to return the next summer having spent the past year just the way they’d spent the school year before–being couch potatoes and eating poorly… and putting on weight.
When I was 17, I was an exchange student in Spain. During my year there, I was fortunate enough to have a personal trainer who helped me change the way I looked at exercise and fitness. At the same time, the family I lived with shied away from fast food and focused on healthy Mediterranean-influenced, balanced meals. The transformation was incredible–I had more energy, strength, and confidence than I’d ever had in my life.
This, combined with further experiences with food and exercise, has shown me not only the value and benefits of a healthier lifestyle, but that much of what’s standing in the way of others’ living such a healthy lifestyle is lack of education and poor habits. It’s for these reasons, I’ve decided to investigate the subject of childhood obesity for potential project opportunities this semester in Designing Meaningful Interactions.
A Brief Overview of Childhood Obesity in the US
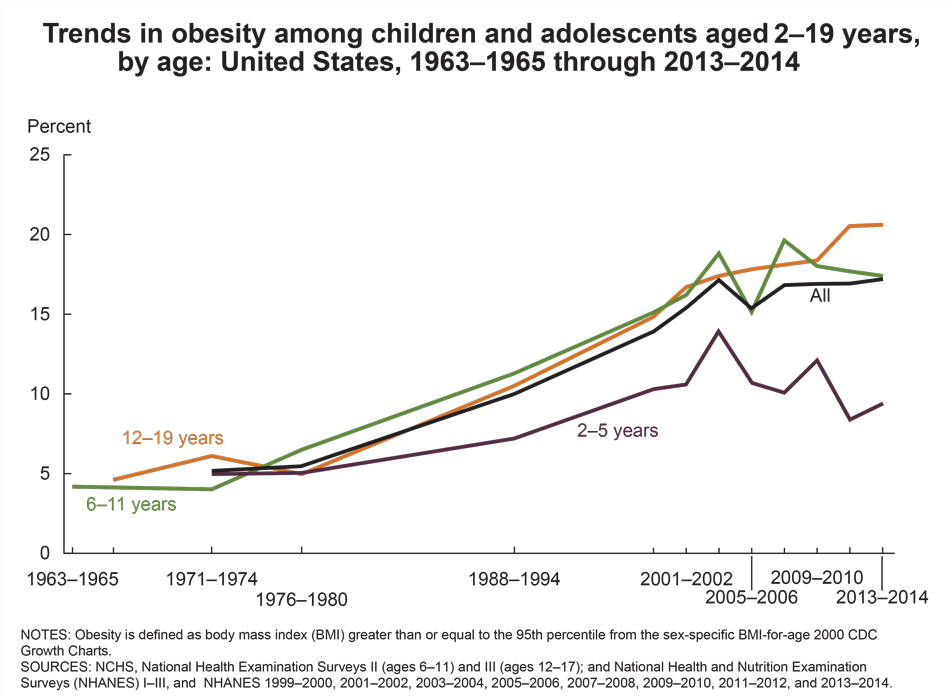
Specifically, the CDC reports that the prevalence of obesity among the listed groups as increasing with age, as follows: 2- to 5-year-olds – 13.9%, 6- to 11-year-olds – 18.4%, and 12- to 19-year-olds – 20.6%. Furthermore, a closer examination of how the prevalence breaks down by race shows significant range: Hispanics – 25.8%, non-Hispanic blacks – 22.0%, non-Hispanic whites 14.1%, and Non-Hispanic Asians – 11.0%. This disparity is something potentially worth looking more closely into when identifying project ideas.
Also from the CDC’s website, regarding obesity and socioeconomic status:
- The prevalence of obesity decreased with increasing level of education of the household head among children and adolescents aged 2-19 years.
- Obesity prevalence was 18.9% among children and adolescents aged 2-19 years in the lowest income group, 19.9% among those in the middle income group, and 10.9% among those in the highest income group.
- Obesity prevalence was lower in the highest income group among non-Hispanic Asian and Hispanic boys.
- Obesity prevalence was lower in the highest income group among non-Hispanic white, non-Hispanic Asian, and Hispanic girls. Obesity prevalence did not differ by income among non-Hispanic black girls.
Why does this matter?
I mentioned earlier why this issue matters to me, personally. Let’s look at what some experts have to say…
National Collaborative on Childhood Obesity Research (NCCOR) has said that “childhood obesity alone is estimated to cost $14 billion annually in direct health expenses, and children covered by Medicaid [read: children of poorer families] are nearly six times more likely to be treated for a diagnosis of obesity than children covered by private.” NCCOR’s site also states that obese children miss significantly more school more than children of average weight, missing over 20% more school days on average. Such absenteeism can have impactful negative effects on a child’s education.
Here are some more facts to chew on childhood obesity’s effects. According to health.gov:
- Long-term, serious health concerns can develop from being obese as a child; among these medical conditions are bone and joint problems, type II diabetes, asthma, heart disease, cancer, high blood pressure, and asthma.
- The effects of early obesity can be more than just physical; early studies indicate that low self-esteem due to childhood obesity likely has negative effects on academic performance and social interactions.
- Research shows obesity in childhood can be tied to obesity later in life; obese children and adolescents are more likely to become obese as adults compared to non-obese children.
- It’s a growing (pun-intended) problem in our country; between 1985 and 2015, the rate of prevalence of obesity in children tripled.
- Among African American and Hispanic youth in the US, the numbers are particularly high; close to 40% are either overweight or obese.
Potential Areas for Involvement and Further Research
In terms of ideas for potential opportunities for creating solutions to chip away that this troubling issue, they include projects which involve:
-parent-/family-involvement (education, group activities, promotion of events & products tie-ins)
-fitness (not weight-loss)-exercise-focused approach
-nutrition-focused approach
-combined nutrition/exercise approach
-wholistic approach (including meditation)
-the creation of a “scouts”-type organization (with heavy tech organization skills)
——-
-app-based customized programs (smartphone, Wii-type games)
-partnerships with local schools and churches/religious organizations…
-even partnerships with:
-
- gyms
- local sports teams
- WW
- REI
- scouts groups
- Let’s Move-type organization? (Also, could look into why it seems Let’s Move had mixed results… and what worked/didn’t work for them as a potential case study.)